Insulin Not Working? It Might Be Time to Change Your Injection Site
Written by: Jodi Lavin-Tompkins MSN, RN, BC-ADM, CDCES
5 minute read
May 13, 2026
Why should you change your insulin injection sites? Get your answer in our Ask a Diabetes Care and Education Specialist (DCES) column!
It’s easy to fall into the habit of using the same spot for insulin injections, especially if it feels comfortable or convenient. But repeatedly injecting into the same area can affect how well insulin is absorbed and make blood sugar management more difficult over time.
If insulin doesn’t seem to be bringing blood sugar down like it used to, injection sites may be part of the problem. Regularly rotating your injection sites can help insulin work more effectively and lower the risk of complications like lipohypertrophy, a buildup of fatty tissue under the skin caused by repeated injections in the same area.
A certified diabetes care and education specialist (CDCES) from the Association of Diabetes Care and Education Specialists (ADCES) shared why site rotation matters and how to choose injection sites that support more consistent insulin absorption.
Why Rotating Insulin Injection Sites Matters
When you first learned to take insulin, the importance of site rotation may or may not have been emphasized. But regularly changing injection sites can make a major difference in blood sugar management.
Changing sites can mean:
- Moving from the stomach to the arm to the thigh
- Moving at least one inch away from the last injection in the same area of the body
What happens when insulin is injected in the same spot?
Insulin causes the fat cells in the tissue of the injected site to grow. Over time, extra fat may develop in the areas where insulin is injected most often. Too much of this fat can prevent insulin from being absorbed normally. This condition is called lipohypertrophy.
Giving injections in the same general area can also lead to numbness in that area. It may become more comfortable and less painful to inject there, but this is often a sign that lipohypertrophy has developed.
Lipohypertrophy can lead to:
- Insulin not being able to be absorbed normally, which leads to higher blood sugar levels
- The need to increase insulin doses over time in order to achieve blood sugar targets
- Higher financial costs due to increased insulin needs
- A higher risk for hypoglycemia when moving injections to a new site because the higher dose of insulin is absorbed optimally in the new area
How to recognize lipohypertrophy
The type of fat that develops with lipohypertrophy is different from the fat associated with weight gain. Signs and symptoms of lipohypertrophy include:
- A1c steadily going up
- More ups and downs with blood sugar levels
- Needing to increase insulin doses without changing a usual routine
- Raised and circular frequent injection sites, often the size of a small orange
It may help to look in the mirror from both the front and side views to see affected areas clearly. If it’s difficult to picture what lipohypertrophy looks like, chipmunk cheeks are often used as an example for the common size and shape, like in the the picture below.
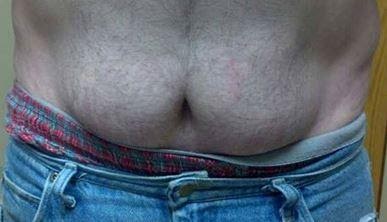
Lipohypertrophy can be mild, moderate, or severe. Mild cases may be more difficult to see, but injection habits can offer important clues.
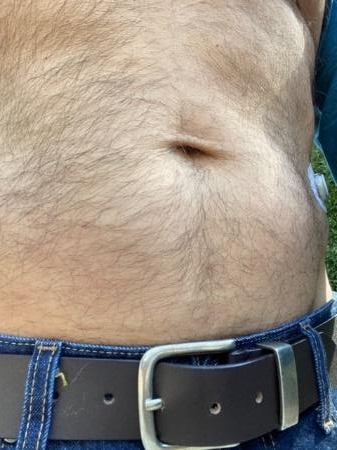
For example, people who often wear untucked shirts may commonly inject on either side of the belly button because it’s easier to access by simply lifting or unbuttoning a shirt.
Below is an example of someone who has only taken insulin for six months but is primarily injecting in those areas of the stomach and has mild lipohypertrophy. One side may have more fatty tissue than the other because if someone is right-handed, it is often easier to inject on the right side, and vice versa.
Preventing and treating lipohypertrophy
Research has shown that reusing pen needles contributes to lipohypertrophy. Most pen needles are designed for one-time use and develop microscopic damage with every use. This can promote injury to the tissue with each injection, even if you can’t feel it.
Lipohypertrophy may go away, but it can take weeks or months. Avoiding affected sites may help them shrink at least somewhat over time.
Insulin absorption varies by injection site
Insulin absorption differs depending on where it’s injected on the body. The best absorption happens when insulin is injected into the stomach area, followed by:
- Arms
- Thighs
- Buttocks
It’s also best to avoid injecting into muscle because it changes the action of the insulin.
What’s the best way to change sites?
The best method is whatever works best for you and helps you remember where you gave your last injection. Some people find that thinking of the body area you are using as a clock helps. Give the first injection at 12 o’clock, the second at 3 o’clock and so on. Others use imaginary lines going across the site and then moving down to the next imaginary line in a horizontal pattern.
Others have gotten creative and developed their own patterns. It’s still better to use the areas outlined in the figure below for the best absorption. You’ll also want to avoid injecting into scar tissue or areas where you can’t pinch an inch.
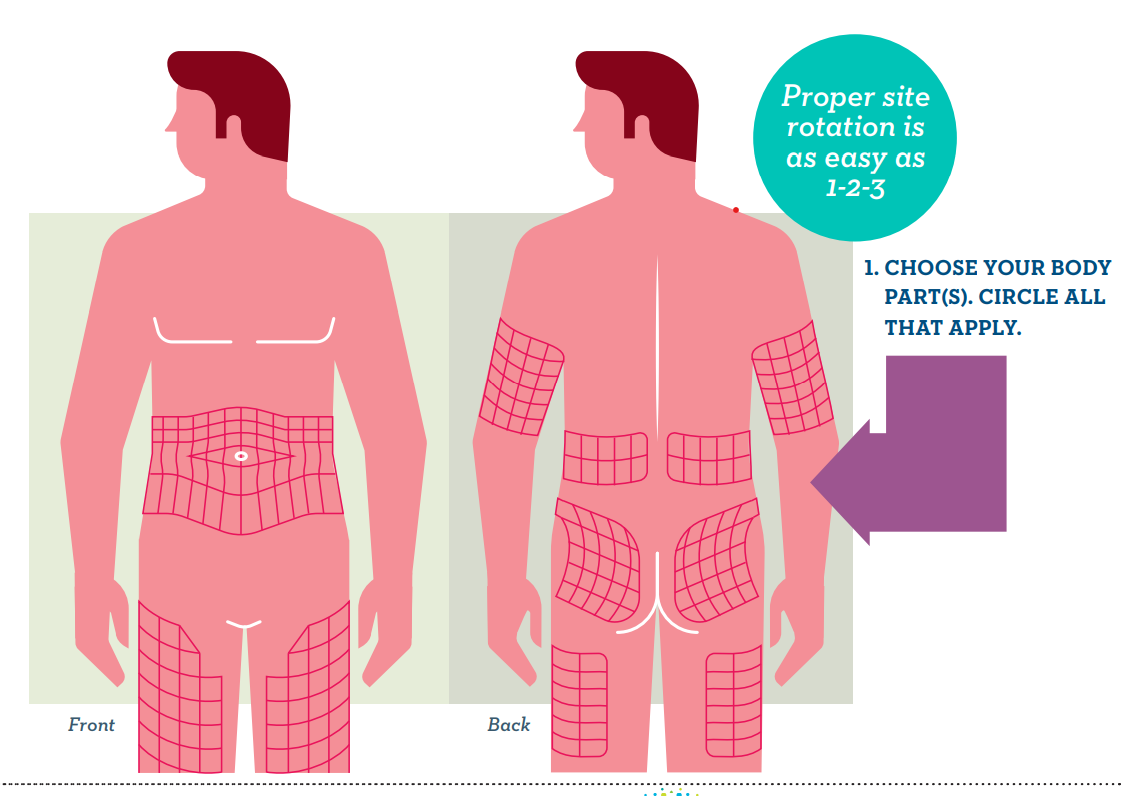
The bottom line
If insulin is part of a diabetes management routine, rotating injection sites, using as much of the entire injection area as possible and changing the needle for each injection can help prevent lipohypertrophy from developing. These small habits can help reduce frustration, improve insulin absorption, and support blood sugar management over time.
Editor’s Note: This content was published in partnership with the Association of Diabetes Care and Education Specialists (ADCES), a founding partner of Beyond Type 2.

Author
Jodi Lavin-Tompkins MSN, RN, BC-ADM, CDCES
Jodi Lavin-Tompkins is a North Carolina native and a master’s prepared nurse with over 30 years’ experience in diabetes care. She is currently the director of accreditation/content development at the Association of Diabetes Care & Education Specialists. Jodi’s career has spanned working in academic settings as a nurse practitioner to positions in the pharmaceutical and medical device industries, to managing a diabetes self-management education and support program in a large midwestern health system. She is passionate about making sure people with diabetes have the knowledge and skills they need to manage diabetes to the best of their abilities. To Jodi, diabetes is personal; her mother, father, brother, niece, cousin, aunt and uncle all have diabetes.
Related Resources

Editor’s note: This article includes Ginger’s personal experience taking metformin in addition to her daily...
Read more

Health insurance can be a headache, especially when selecting a plan that will cover the...
Read more

You may need to switch your type 2 medications at some point in the year....
Read more