Ask a DCES: Dawn and Somogyi Effect: Morning High Blood Sugars Explained
Do you ever wish you could ask a diabetes care and education specialist (DCES) anything about type 2 diabetes? In our new monthly Ask a DCES column, you can get your most burning questions answered from a DCES professional on various topics, including diet, medication, exercise and mental health. Want to submit a question to us? Email us at hello@beyondtype2.org!
Dear DCES: I have noticed that I go to bed with my blood sugar looking good but I wake up with much higher blood sugar than I expected. Why is this the case?
Dear Reader: I know waking up with higher-than-expected blood sugars can be frustrating for you. There could be various reasons for this, but I am going to focus on two common ones. 
The first one is known as the Dawn Effect. Everyone has a body clock that responds to daytime and nighttime. When dawn arrives and the sun starts to come up, your body reacts by secreting hormones (growth hormone, cortisol, glucagon and epinephrine) that get you “ready for your day.” These hormones cause a rise in blood sugar that is harder for your body to compensate for if you have diabetes.
Another cause of higher morning readings is the opposite of the dawn effect, called the Somogyi Effect, but the end result is the same; higher than expected blood sugars in the morning. In this case, the cause of the rise in blood sugar in the morning is the result of having a low blood sugar overnight, known as “nocturnal hypoglycemia”. Symptoms of nocturnal hypoglycemia may include restless sleep, nightmares and sweating. This may be caused by too much basal insulin or the effects of exercise, for example. Whatever the reason, your body responds to the low blood sugar with similar hormones that lead to the dawn effect. But the rise in blood sugar is due to your body responding to raise your blood sugar to a safer level; some people refer to it as a “rebound” high blood sugar.
How do I know if high morning readings are due to the Dawn Effect or the Somogyi Effect?
The best way to find out is to do some overnight monitoring. Here are some overnight monitoring tips steps to identify if your high morning blood glucose is due to the Dawn Effect or Somogyi Effect:
- Start your overnight checks at least three-to-four hours after your last meal
- Refrain from eating during the overnight check unless you need to treat a low blood sugar. Avoid drinking alcohol.
- In the middle of your sleeping cycle. For example, if you sleep from 11pm to 7am, you would check around 3am. If you skip this step, you will not have enough information to sort out what is happening.
- If you use a continuous glucose monitor, check your overnight history in the morning
The results of your overnight check should reveal whether you are experiencing the dawn or the Somogyi effect. You may need to repeat your overnight monitoring one or two times to confirm.
Dawn Effect vs. Somogyi Effect
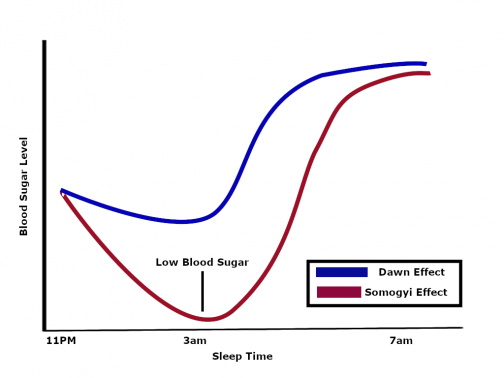
How to Correct High Morning Blood Sugar
Because the causes of the Dawn and Somogyi effects are different, your problem-solving approaches for both of them need to be different. Here are some approaches to solve your morning highs:
For the Dawn Effect:
Try a bedtime snack: It is reasonable to experiment with having a bedtime snack to see if it helps prevent the unexpected rise later in the morning. You can also experiment with the type of snack, altering the amounts of fats, carbohydrates and proteins to see if the effects are different.
Eat regularly: Don’t go for more than six hours without eating. The longer you go without eating, the more likely your body will perceive this as a problem and try to use its own energy stores, which contributes to the higher readings.
Eat dinner earlier: Lengthening the amount of time between dinner and bedtime gives your body more time to get your blood sugar down after eating. Eat dinner earlier if you can.
Be active after dinner: Any activity helps to lower blood sugar. Do a light physical activity after dinner may be helpful.
Take medications consistently: Some diabetes medications that are commonly prescribed act by helping with the rise in blood sugar from hormone effects overnight, so being sure not to miss any medication doses will help. Set an alarm if you need help remembering.
Discuss your medication timing and dosage with your provider: Ask if the timing of your medications in relation to your meals is optimal. There may be an option to move a dose that helps with the Dawn effect. If you are using an insulin pump, your overnight basal rate can be adjusted to blunt the rises in blood sugar in the early morning hours. Your morning dose of medication may be increased to account for this rise in morning blood sugar.
For the Somogyi Effect
Count carbs: Be as consistent as possible with your carb servings at night.
Eat regularly: Skipping meals can lead to low blood sugar if you are taking diabetes medications.
Avoid alcohol, but if you drink it be sure to eat a snack: Some people are very sensitive to alcohol and may need to eliminate or reduce it to avoid low blood sugars. Drink in moderation.
Think about the timing of your activity/exercise: Is evening activity causing your blood sugar to go low overnight? If so, work out earlier in the day.
Adjust insulin to carb ratio: If you are carb counting, you may need to consult your diabetes care team to better match your meal insulin to your carb amounts.
Discuss your medication timing and dosage with your provider: It’s important to understand the actions and effects of all of your diabetes medications and take them at the recommended times. If you take basal insulin, you may need to discuss adjusting your dose with your healthcare team.
For more information on how a Diabetes Care and Education Specialist can help you manage your blood sugar, visit diabeteseducator.org/DCEShelp.
This content was produced in partnership with the Association of Diabetes Care and Education Specialists (ADCES), a Founding Partner of Beyond Type 2.





