Should I Ask My Primary Care Provider for Glucagon?
Written by: Ginger Vieira
6 minute read
March 10, 2026
Es posible que tu médico no sepa sobre glucagon de emergencia, por qué lo necesita y los tipos más nuevos disponibles. He aquí cómo solicitarlo ...
If you use insulin or another blood-sugar-lowering medication to manage your diabetes, you should have an emergency glucagon with you. It doesn’t matter what your A1C is or whether you’ve never had severe low blood sugar (hypoglycemia) before.
Diabetes doesn’t play fair and often comes with a lot of unexpected bumps, no matter which type you have. You should have an emergency glucagon—period.
Primary care providers don’t always know about glucagon
Many people with type 1 and type 2 diabetes may not always have regular access to endocrinologists, who are experts in treating different kinds of diabetes. Often, they visit a primary care doctor instead.
Your main doctor might not know all the types of glucagon available today. That’s why it’s important to come to your appointment prepared with questions and some knowledge. This will help you speak up for what you need and ensure you get the type of glucagon you prefer.
You may also ask for a prescription for emergency glucagon that your insurance covers. Sometimes, your preference and what insurance will pay for might not be the same. It’s a good idea to ask your doctor about this, which we’ll discuss below.
Before you start asking about an emergency glucagon prescription, let’s go over the basics of what glucagon is and how it works.
Emergency glucagon 101: what is it?
Glucagon is a hormone that tells your liver to release stored sugar, called glycogen, into your blood. Emergency glucagon shots can help raise your blood sugar during severe hypoglycemic episodes when your blood sugar falls to 55 mg/dL (3.1 mmol/L) or lower.
While there was only one option for decades—and it was complicated to use—there are many new and improved emergency glucagon treatment products available today, including:
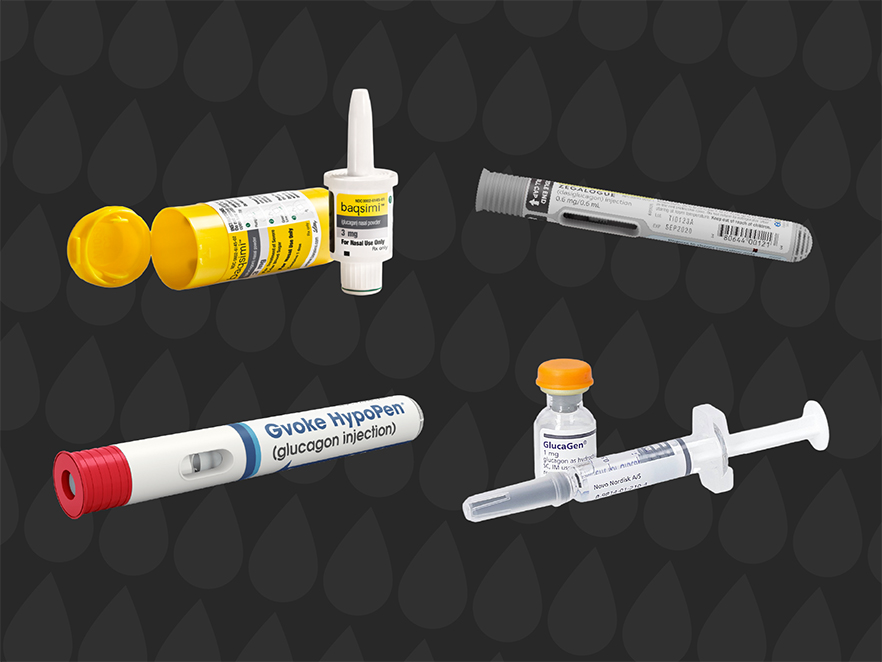
- Nasal glucagon—Baqsimi®: This is an emergency glucagon that’s administered through your nose.
- Glucagon pen—Gvoke HypoPen®: This is a premixed glucagon injection that you press against your thigh. The auto-inject device makes it quick and easy to use. It is also available in a prefilled syringe (PFS).
- Glucagon Prefilled Syringe—Gvoke Kit®: This is a premixed glucagon in a vial that comes with a syringe, allowing you to draw up the dose manually and inject it directly into your thigh.
- Glucagon pen—Zegalogue®: Also a premixed glucagon, available as an easy-to-use auto-inject device. It is also available in a prefilled syringe (PFS).
Why is it important for people with diabetes to get glucagon?
The longer you live with diabetes, the higher your risk of having severe low blood sugar. This can happen because your body might stop telling you when your blood sugar is too low, which is called hypoglycemia unawareness. This isn’t always the case, but it isn’t uncommon either.
As you get older with diabetes, your body experiences more changes. Just a little more insulin than your body needs can cause a serious low blood sugar. If you have diabetes and use insulin, low blood sugar is often hard to avoid, even if you try to prevent it.
Most low blood sugar can be fixed with 15 grams of fast-acting carbs, such as hard candy or juice, then waiting 15 minutes. But one severe case of low blood sugar can cause a seizure or other life-threatening complications.
You might go years without needing an emergency glucagon, but it’s a good idea to be proactive and have it on hand just in case.
Emergency glucagon could save your life in situations when:
- You’re unconscious and can’t eat or drink fast-acting carbs like glucose tablets, powders, gels or gummies, hard candy, soda, juice, etc.
- You’re having a seizure. You’re vomiting excessively and can’t consume carbs
- You accidentally took too much insulin or took the wrong kind of insulin
- You’restill conscious but feel like you’re going to pass out.
Usually, a friend or family member can administer emergency glucagon if you’re unconscious or having a seizure due to severe low blood sugar. It’s important to tell family and friends where your glucagon is stored and to train them on how to use it on you.
How to ask your doctor for an emergency glucagon
You can ask for an emergency glucagon prescription the next time you see your doctor by leaving a message on the phone or through your online health account. It’s not a big deal and doesn’t need any extra tests.
If you take insulin, your doctor should agree that it is a critical tool for safely managing diabetes.
Will my insurance cover glucagon?
Everyone’s insurance is different. That means you might need to follow different rules depending on your insurance, your diagnosis and how you’re taking care of your health. Don’t worry about this. Just be aware so you can stay calm and know what to do next if it happens to you.
Insurance can be finicky, but you will always learn with new prescriptions, so the next time it will be easier. Your healthcare team can support you through this if it happens.
Reasons for emergency glucagon insurance denial may include:
- Formulary exclusions or preferred alternatives: A formulary is a list of brand-name and generic medicines that your insurance will pay for. If a medication isn’t on your insurance’s list, it means your insurance recommends a different drug.
- Prior authorization needed: Prior authorization is the approval from your health insurance needed for a service, treatment or medication to be paid for by your plan in non-emergency situations. Insurance may require prior authorization when your doctor requests a prescription.
- Administrative errors: Or better known as clinical office errors. eople make errors because healthcare is still human. Mistakes in paperwork often lead to automatic denials.
If your health insurance says no to paying for your prescription, don’t worry. Call them to find out why. Talk to your doctor about next steps. Don’t just accept the first no. An emergency glucagon should be a part of your diabetes toolbelt—no questions about it.
Patient assistance programs (PAPs) and copay cards can also help people get emergency glucagon more affordably, which can still be costly even if insurance covers it.
Why doesn’t my doctor already know about glucagon?
You might need to explain to your doctor why a person with diabetes who takes insulin or other blood-sugar-lowering medication needs emergency glucagon. While this may feel overwhelming, don’t get discouraged.
Stay positive and remember that everyone on your healthcare team is part of many other teams as well. Your health is important, and no one knows your personal story better than you. You may need to share more of your history to help them remember or have a better conversation.
Remember: your healthcare provider is on your team and wants what’s best for you. Sometimes, you just have to tell them what that is (kindly and respectfully) during your visits.
Are you passionate about raising awareness of the signs of diabetes? Become a #SeeTheSigns ambassador! Join the global movement with a simple message to see the signs of diabetes.
Related Resources
Low blood sugar can make people with diabetes (PWD) feel exhausted, frustrated and scared. Sometimes,...
Read more

Sensitive Topic Warning: For some people, eating a lot of food all at once when...
Read more
You’ve probably heard of the EpiPen and how it can save someone’s life if they’re...
Read more


