Beyond Type 3c?: A Pancreatitis Diabetes Diagnosis
Written by: Robert Valdez
6 minute read
July 10, 2019
Beyond Type 3c? That's how Robert Valdez is living. He was diagnosed with pancreatitis-induced diabetes in 2019. He also suffers from a spinal cord that impacts his diabetes care. Read his story here.
Robert Valdez originally thought he had type 2 diabetes, but a recent diagnosis revealed otherwise. Read his story below. Robert has also been featured in our #BeyondPowerful social media campaign. To be featured in the campaign, click here!
My name is Robert Valdez and I reside in Houston, Texas. I am 40 years old and I was diagnosed with diabetes in 2014 after having gallstone pancreatitis—known as type 3c diabetes. In 2012, I was admitted to the hospital for gallstone pancreatitis which was caused by a gallstone blocking my pancreatic duct and had surgery to remove my gallbladder and gallstone. On admission, I was at my heaviest weight at 330 lbs (150 kg). Throughout the year, I was in and out of hospitals because of the constant flare-ups from pancreatitis and was often admitted for pain management and dehydration. Because of this, I lost almost 100 lbs (45 kg) and dealt with severe depression. Later on, a former emergency room physician and colleague told me about the links between pancreatitis, diabetes and pancreatic cancer.
and was often admitted for pain management and dehydration. Because of this, I lost almost 100 lbs (45 kg) and dealt with severe depression. Later on, a former emergency room physician and colleague told me about the links between pancreatitis, diabetes and pancreatic cancer.
I started to experience the usual symptoms associated with diabetes such as frequent urination, rapid weight loss and increased thirst. I found out I had diabetes on my birthday. My blood glucose levels were pushing 33.3 mmol/L600 mg/dL. The first medications I were prescribed were Metformin and Lisinopril. Later on, I was prescribed Jardiance and Farxiga because metformin wasn’t effective enough. This combination helped bring my blood sugar down to normal ranges. Unfortunately, a change in health insurance plans caused a lapse in coverage of Jardiance and Farxiga. However, I was able to use Glimepiride and have seen positive results.
From Pancreatitis to Diabetes
It wasn’t until 2017 that I decided to take some part of my life back. I decided to get physically fit and closely manage my diabetes. I was fortunate to have found a primary care physician who was willing to work with me in the treatment of my diabetes. Even though I saw a diabetes educator and nutritionists, those visits weren’t enough—I needed more help.
On January 23rd, 2019, I sought the help of an online coach with meal plans and exercise routines to help me lose additional weight. I did an eight-week plan that lasted until March 19th. My goal for this program was to be better educated about meal portion sizes and the exercises for specific muscle groups, as well as new tips to help lower my blood glucose levels. The week I started the program, my fasting blood glucose was 13.9 mmol/L250 mg/dL. Since then, my fasting glucose is between 6.1-7.9 mmol/L110-143 mg/dL. I kept a journal of my workouts and glucose levels and posted my journey on Instagram to keep myself accountable and to motivate others.
When I made the decision over two years ago to take control over my diabetes through fitness/nutrition and thinking the issues with pancreatitis was behind me, little did I know it would resurface. In early March I started to experience mid to left abdominal discomfort. During my three month check-up to reassess my A1C’s and expressed to my primary care physician of the concern I was having, he ordered a CT (cat scan) abdomen/pelvis.
On May 7th, 2019 after a CT exam was done, I received a phone call from my primary care doctor stating they had found a pseudocyst within the pancreatic wall and he was making arrangements for me to see a GI specialist (gastrointestinal). Within the week I followed-up with the GI specialists and during the visit, he expressed the symptoms I had been feeling was pancreatitis. Also, with my history of pancreatitis, the type of diabetes I have is known as pancreatogenic diabetes or type 3c. Type 3c diabetes happens when the pancreas has suffered some type of trauma to it. In my case, the trauma that occurred was from having gallstone pancreatitis seven years prior. The treatment for this would be to have an ERCP (endoscopic retrograde cholangiopancreatography) with an endoscopic ultrasound done. During the procedure, they would be placing stents in the pancreas to drain the pseudocyst to help alleviate some of the discomforts I was experiencing.
Before the visit concluded, it was informed I would need to be followed-up with every two to three years to evaluate the pancreas for further damage or if pancreatic cancer would be detected early because of the rarity of type 3c diabetes and how the pancreas was affected. I had the ERCP with the endoscopic ultrasound procedure and in two months the GI specialist will remove the stents and determine when I would need further evaluation.
How a Spinal Cord Injury Affected My Diabetes Management
 For the first three years, I didn’t manage my diabetes well. When someone is diagnosed with diabetes or any disease, there’s usually a change in one’s routine and sometimes denial. I was that person in denial. As a healthcare provider, I knew what the consequences of poorly-controlled diabetes, yet I wasn’t doing much to prevent them.
For the first three years, I didn’t manage my diabetes well. When someone is diagnosed with diabetes or any disease, there’s usually a change in one’s routine and sometimes denial. I was that person in denial. As a healthcare provider, I knew what the consequences of poorly-controlled diabetes, yet I wasn’t doing much to prevent them.
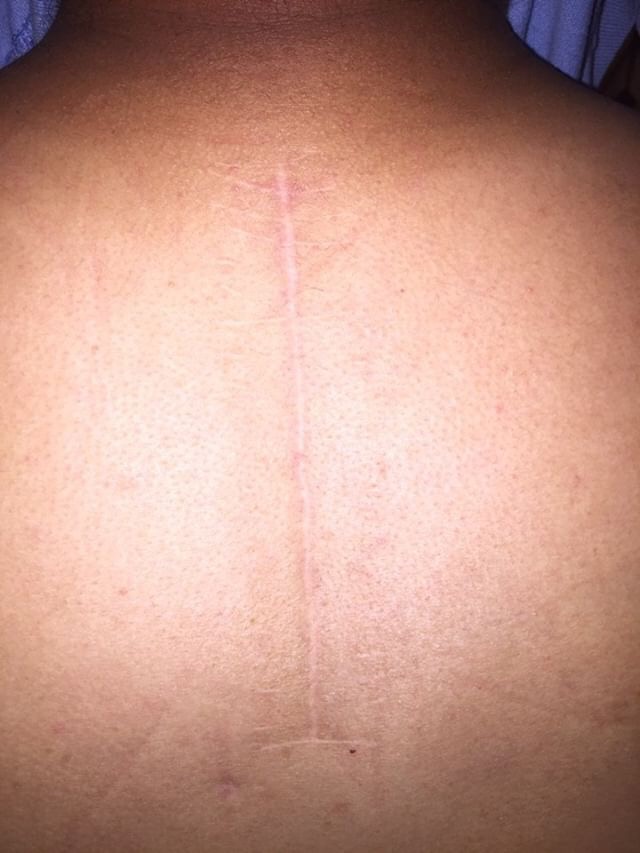
In October 2014, I joined a local gym to lose weight. During that month I noticed sharp pains in my middle back radiating down to my legs. I assumed I had done an improper lift and discontinued those exercises. As the months went by, the pain worsened. Not only did I have numbness and tingling from mid-chest down, but my legs felt as if they were asleep. I was starting to lose all sensation from my lower extremities and gradually, my manner of walking began to slow and eventually, it became difficult to walk. I went to an emergency room and had a cat scan done and the results showed a severe spinal cord compression from T1-T4. The next morning, I was in the operating room having a laminectomy.
Although, I have regained some sensation to my lower extremities after having the back surgery, living with diabetes also complicates the neurological symptoms as well, especially if it’s uncontrolled or my blood sugar is high. When my blood sugar is high, the sensation in my legs is poor. I do daily neuro checks to assess any changes in the feelings of my lower body. This allows me to determine if there are any abnormal sensations.
Working in Emergency Medical Services + Acute Care Gave Me a New Perspective
I started my career as a healthcare provider when I was about 17 or 18 years old. Before 21, I was working in my first emergency room for a level II trauma center. Over the years, I’ve worked as an ER tech and other areas within a hospital. While working in Emergency Medical Services (EMS) I’ve seen countless hospitalizations due to various illnesses and injuries. As a result, I became familiar with the signs and symptoms of diabetes and since I’ve started living with it, I know how to determine if someone is having a diabetes-related emergency.
My experience helps me relate more to my patients. I remember when I couldn’t understand why I’d see some of the same patients and began to understand sometimes it was due to the lack of medication affordability. Other times, it was their lack of care during the holidays. Holidays were notorious for people with diabetes to visit the emergency room who would claim their blood sugar was too high. But, patients would admit to eating foods high in carbs and sugar such as pies, stuffing, or drinking sweet tea. As a response to the high blood sugar, patients would simply say they’d get back on track later.
Empowering Through Education
People with diabetes are taught to know the consequences of good and bad nutrition. We are in charge of what we choose to eat. I have seen the long-term effects of having uncontrolled diabetes and uncontrolled blood pressure on patients and their families.
But, I think people with diabetes could use a more holistic approach to learning about it. For example, I am more aware of the daily condition of my skin. It’s the single most protective layer that prevents infection or harmful substances from entering the body until that protection is compromised. When the skin is compromised, we are prone to infection, which can lead to amputation and prolonged healing as well. However, that’s not the only diabetes complication I’ve seen. Along with patients with amputated limbs, I’ve treated patients who have lost their vision, patients who were on dialysis and have seen them pass away.
At the end of the day, my goal is simple—I want to educate the public not all people with diabetes “look sick.” In fact, many people with diabetes live an active lifestyle. Also, I want to create a program for people with diabetes to receive proper education when diagnosed and improve the relationship between patient and provider. Through proper education, people with type 2 diabetes can feel empowered each day to tackle the disease head-on and reach the goals they set for themselves, including living a healthy and active lifestyle.
[bt1-cta link=”https://beyondtype1.org/robertvaldez/” text=”Join the Beyond Type 2 Community!” color=”blue” align=”left” ]

Author
Robert Valdez
I am a healthcare provider and certified as an emergency medical technician and currently in the process of applying for nursing school. Surf or kayak fishing is a passion of mine when given the opportunity to do them. Also, for vacation, my wife and I enjoy traveling by cruise to places such as the Bahamas, Grand Cayman, Jamaica, and Cozumel.
Related Resources

Danica Collins not only prepared for one of the most challenging physical events of her...
Read more

Beyond Type 1 is spotlighting inspiring athletes with type 1 diabetes as they prepare for...
Read more

On November 3, 2024, Taylor Rindfleisch of Chicago laced up her running shoes for the...
Read more

