Guide: Talking to Your Doctor About Insulin for Type 2 Diabetes
Written by: Ginger Vieira
6 minute read
January 20, 2022
Starting insulin therapy for type 2 diabetes can be overwhelming—there’s a lot to learn! Here are some questions to ask your doctor to help you get started with using insulin.
Whether you’re curious about using insulin or you just started using it, insulin therapy for type 2 diabetes (T2D) can be overwhelming—there’s a lot to learn! But insulin can also help you reach your blood sugar goals, improve your overall diabetes health and protect you from diabetes complications.
Here are some questions to ask your doctor to help you get started with using insulin.
Questions to ask your doctor about using insulin
Insulin is a complicated medication—just a little bit too much or not enough can have a big impact on your daily safety, your blood sugar levels and your overall health. The more you know about insulin, the more you can manage your blood sugars safely!
While there are many medication options for people with type 2 diabetes, if your body needs insulin, it’s important to understand why or how to use it safely.
(Taking a non-insulin diabetes medication? Here’s a guide to talking to your doctor about those, too!)
Why do I need to start using insulin?
Every person on the planet needs insulin in order to live. Without enough insulin, your body cannot use the sugar in your bloodstream for energy. That sugar builds and builds, making you feel sicker and sicker and damaging nearly every major part of your body, including your eyes, toes, fingers, feet, kidneys, liver, stomach—the list goes on and on!
As a person with T2D, your healthcare team may be recommending you start taking insulin for a few reasons:
- If you’ve just been diagnosed and your blood sugars have been dangerously high for a while, insulin is the fastest way to get you down into a safer range. Once things are stabilized, your healthcare team might be able to consider other treatment options.
- If you’ve lived with T2D for a while and tried other options, your healthcare team may have decided that your body isn’t responding well to those non-insulin medications. When other medications aren’t working well enough to help your body use the insulin you naturally produce, insulin therapy is a natural next step to help bring your blood sugars down into a safer range.
- T2D is a “gradually progressive” disease for many people. This means that overtime, your body is producing less and less insulin. At a certain point, it’s time to help your body get the amount of insulin it truly needs to maintain safer blood sugar levels by starting insulin therapy.
How do I take insulin?
Don’t let your appointment end without asking your doctor to show you every single step of taking an insulin injection or inhalation. While it can be quite simple, it’s still important to follow each step carefully and accurately.
Use our step-by-step guide to help you learn the ropes.
I’m scared of needles, how can I manage this while taking insulin?
“Needle-phobia” is a common issue. Who wouldn’t hate taking regular injections? Fortunately, there are options today that help you take your insulin without ever seeing the needle itself—or you can try “inhaled” insulin, too!
You have options! Don’t let needle-phobia keep you from taking the medication your body needs in order to stay healthy and safe.
What kind of insulin am I taking?
Yes. When it comes to insulin, it’s important to ask your doctor whether you’re taking a “mealtime” insulin or a “background” insulin.
- Mealtime insulin: Also known as “bolus” insulin, acts quickly in your system after it’s taken. You should only take it when you are eating a meal or as instructed by your doctor to correct high blood sugars. If you’ve decided you aren’t going to eat lunch, for example, then you shouldn’t take your lunchtime insulin dose.
- Background insulin: Also known as “basal” insulin, it stays in your body for anywhere from 12 to 36 hours depending on the type you’re taking. This type of insulin helps your body manage your blood sugar even when you’re not eating. It’s important to take this insulin every day as your doctor instructed, even if you are sick or skip a meal or you’re traveling or—whenever!
If you have any concerns about taking insulin, tell your doctor. If you are experiencing frequent high or low blood sugars, tell your doctor immediately.
How do I know if I’m getting too much insulin?
Low blood sugars are the sign that you’re getting too much insulin. A mild low blood sugar between 55 to 80 mg/dL can result in symptoms like feeling sweaty, shaking, light-headed, hungry and weak.
If you take insulin, you should always carry fast-acting carbohydrates with you—like jelly beans, juice, or glucose tabs—to treat low blood sugar. Most lows can be treated with 15 grams of carbohydrate.
Severe low blood sugars, lower than 55 mg/dL, can potentially lead to seizures, coma, or death. Everyone who takes insulin should emergency glucagon. If you feel unable to manage the low blood sugar on your own, call 911!
How do I know if I’m not getting enough insulin?
High blood sugars are the sign that your body isn’t getting the amount of insulin it needs to maintain safe, healthy blood sugar levels.
Symptoms of high blood sugars include craving sugar, blurry vision, feeling thirsty, feeling tired and feeling irritable.
Using your glucose meter or continuous glucose monitor (CGM), you can check your blood sugar at certain times of day to determine if you’re in your goal ranges. If not, talk to your doctor about adjusting your insulin doses and other medication doses.
What could potentially cause my body to need less insulin?
Whether you have any type of diabetes or not, you can take steps to improve your body’s sensitivity to insulin and reduce your overall insulin needs. Insulin resistance can lead your body to needing more insulin.
For some people, this can lead to no longer needing to take insulin via injection or inhalation. For others, it can help improve your blood sugars and reduce your insulin doses while still needing insulin to manage safe blood sugar levels.
The simplest habits can lead to a big impact on your sensitivity to insulin, including:
- Getting at least 30 minutes of low-impact exercise a day (like walking)
- Getting 30 minutes of strength-training a few days a week
- Losing weight
- Reducing the amount of sugar you consume in food or drinks
- Increasing your overall daily activity level (even just getting up from your work desk every hour)
- Quitting smoking
- Reducing your alcohol intake
Talk to your doctor about working with a dietitian or certified diabetes care and education specialist to help you work on gradual improvements in your daily lifestyle habits!
How long will I need to take insulin for?
Some people with type 2 diabetes may need to take insulin for the rest of their lives—even if you have healthy lifestyle habits that keep insulin resistance at bay. Some people with type 2 diabetes may only need insulin for a few months or years as they work on other changes in lifestyle habits or are able to transition to non-insulin medications.
For many people, T2D is a “gradually progressive” disease which means your body produces less and less insulin every year. For others, it can be eventually managed through weight-loss, diet changes and daily exercise.
Regardless, every human on the planet can work to help their body need less insulin through healthy lifestyle habits that improve your body’s sensitivity to insulin. Talk to your doctor about what might be a reasonable expectation for you and your diabetes.
Insulin is expensive! What if I can’t afford it?
Insulin is very expensive. Fortunately, there are a few resources available today depending on your insurance or income status, to help you get the insulin you need.
Visit either of these resources to help you afford your insulin:
Your healthcare should also be helping you navigate the different resources to help you afford your insulin. If you’re having trouble, talk to your doctor and healthcare team immediately!
I don’t like taking insulin, can I stop taking it?
No, you should not stop taking your insulin. Insulin therapy is not easy—even if it does help us protect your eyes, toes and kidneys from diabetes! But you shouldn’t stop taking it without discussing this carefully with your doctor.
Some people will need to continue taking insulin for the rest of their lives. Some people may be able to lessen their need for insulin therapy through making changes in lifestyle habits and using other types of diabetes medications.
Suddenly stopping your insulin can lead to dangerously high blood sugar levels that threaten both your immediate and long-term health and safety!
If you’re unhappy with your insulin regimen or side-effects you’re experiencing, contact your healthcare team immediately.
If you believe you’re experiencing frequent or severe low blood sugars, check your blood sugar, treat the low with fast-acting carbohydrates or emergency glucagon or call 911—and reach out to your healthcare team immediately to discuss your overall insulin regimen.
Educational content related to type 2 diabetes is made possible with support from Lilly Diabetes, an active partner of Beyond Type 2 at the time of publication. Beyond Type 2 maintains full editorial control of all content published on our platforms.

Author
Ginger Vieira
Ginger Vieira is an author and writer living with type 1 diabetes, celiac disease, fibromyalgia and hypothyroidism. She’s authored a variety of books, including “When I Go Low” (for kids), “Pregnancy with Type 1 Diabetes” and “Dealing with Diabetes Burnout.” Before joining Beyond Type 1, Ginger spent the last 15 years writing for Diabetes Mine, Healthline, T1D Exchange, Diabetes Strong and more! In her free time, she is jumping rope, scootering with her daughters or walking with her handsome fella and their dog.
Related Resources
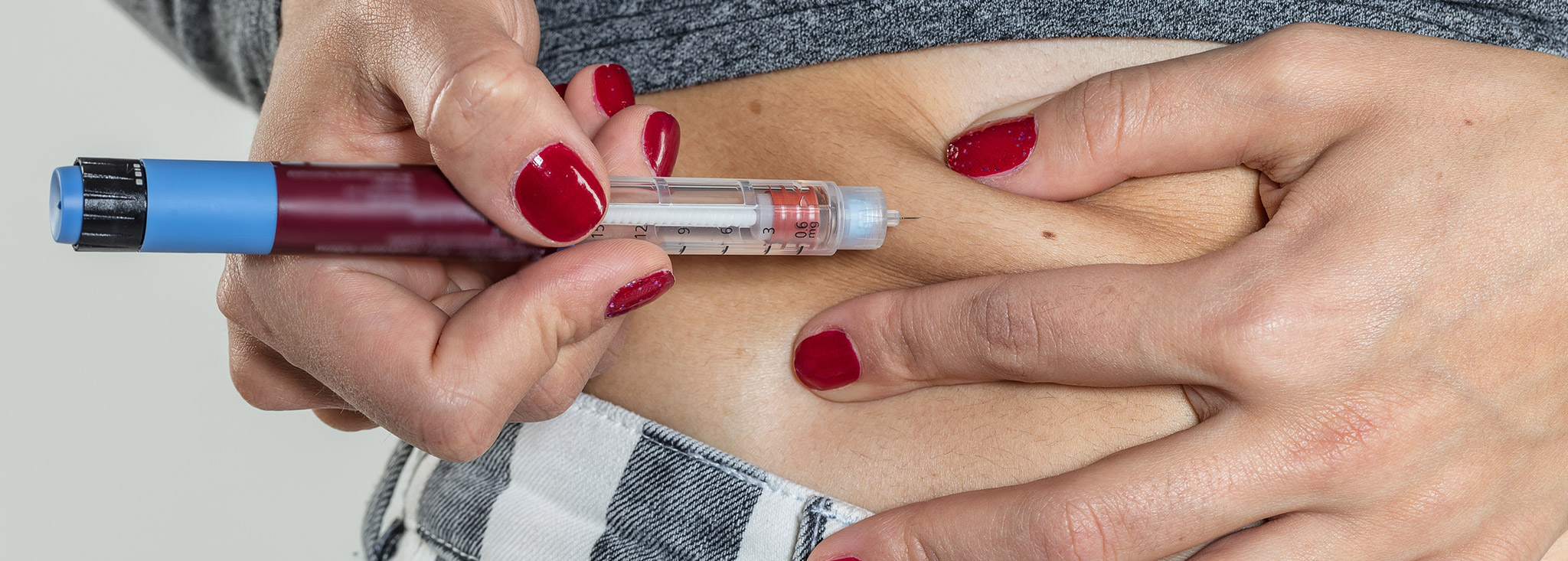
It’s easy to fall into the habit of using the same spot for insulin injections,...
Read more

Managing type 2 diabetes means keeping your blood sugar levels within a healthy range and...
Read more

Physical activity plays a crucial role in managing diabetes, and walking is an easy, effective...
Read more

