When Medications are Prescribed for Type 2 Diabetes Management
Written by: T'ara Smith, MS, Nutrition Education
6 minute read
January 29, 2021
Doctors follow a set of protocols to determine when to recommend medications to T2D patients. Learn when they're likely to prescribe them.
When you’re newly diagnosed with type 2 diabetes (T2D), you may be wondering if or when you’ll need medication to manage it and which medications are available to you. Fortunately, there’s a protocol listed in the American Diabetes Association’s 2021 Standards of Care that health care professionals follow to determine when and what kinds of medications are recommended to help you reach your glycemic goals. In this article, we’ll list the drugs indicated for type 2 diabetes management, as well as when and how doctors are guided towards making the choice to recommend them to patients.
Medications for Type 2 Diabetes Management
- Metformin (Biguanides)
- Basal Insulin (Long-acting insulin)
- Bolus Insulin (Mealtime/rapid-acting/prandial insulin)
- Mixed Insulin
- Sulfonylureas
- Thiazolidinediones (TZDs)
- Dipeptidyl Peptidase-4 (DPP-4) Inhibitors
- Sodium-Glucose Cotransporter 2 (SGLT-2) Inhibitors
- Glucagon-Like Peptide-1 (GLP-1) Receptor Agonists
- Glucagon
How Doctors Determine When to Prescribe Medication
Metformin
The first line of treatment for type 2 diabetes is with metformin, along with lifestyle modifications. Although metformin’s side effects include gastrointestinal issues such as bloating, abdominal discomfort and diarrhea, this drug is safe and inexpensive and the side effects can be lessened when metformin is taken gradually.
Combination Therapy
It’s important to remember that type 2 diabetes is a progressive chronic illness, so the treatment with metformin may only work for a few years until another medication is added, at no fault of the patient. Combination therapy allows for patients to reach their A1C targets and sustain their progress.
When A1C is 1.5 percent or more above target, most patients will require some sort of combination therapy, in other words, taking metformin with another medication. In this case, a doctor may prescribe insulin in patients with blood glucose levels at or above 16.6 mmol/L300 mg/dL or an A1C above 10 percent (86 mmol/mol), or if the patient is experiencing hyperglycemic symptoms such as polyuria and polydipsia (frequent urination or thirst) or weight loss. Doctors may also recommend a sulfonylurea.
The Standards of Care advises health care professionals not to delay discussing the combination therapy strategy when treatment goals aren’t being met. The choice of intensifying treatment depends on the preferences of the patient and the progress of their diabetes management, including other health and socioeconomic factors such as:
- Cardiovascular diseases
- Chronic kidney disease
- Other comorbidities
- Cost
- Potential side effects, safety and tolerability
Also, if a patient isn’t reaching their target goals within three months, metformin can be combined with any of these six treatments:
- Sulfonylureas
- Basal Insulin
- TZDs
- DPP-4s
- SGLT-2s
- GLP-1 RAs
When Medications are Prescribed for Patients with Type 2 Diabetes and Cardiovascular Disease or Chronic Kidney Disease
For patients who are 55 years old or older who have or are at high-risk for cardiovascular diseases (CVD) and chronic kidney disease (CKD), an SGLT-2 or a GLP-1 is recommended independently of A1C or metformin use. These drugs have displayed benefits for patients with CVD and CKD.
For patients who aren’t at risk or have a history of CVD or CKD, the decision to add a second (or third) drug to the treatment with metformin is based on efficacy, avoidance of side effects such as hypoglycemia and weight gain, cost and the patient’s preferences.
How Insulin is Prescribed
Unfortunately, people within the type 2 diabetes community have been threatened with the prescription of insulin or see the start of insulin therapy as a sign of failure of managing diabetes. But, insulin therapy is an effective way to manage type 2 diabetes and the start of it is never the patient’s fault, but just a sign of type 2 diabetes (T2D) progression. With that said, it’s important for health care professionals to continually explain the progression of type 2 diabetes.
The kinds of insulins available are:
- Basal (long-acting) insulin
- Bolus (meal-time or rapid-acting) insulin
- Concentrated insulin
- Inhaled insulin
Basal Insulin:
Basal insulin regulates blood glucose overnight and between meals and lasts for 24 hours. This kind of insulin can be added to metformin or used alone. Starting doses are estimated based on body weight, the intensity of hyperglycemia and trial and error based on the patient’s experiences.
Mealtime Insulin:
Mealtime insulin, also called rapid-acting or prandial insulin, are taken before meals and in addition to basal insulin. To start, a doctor may recommend a dose of four units or 10 percent of the amount of basal insulin and adjust it according to the patient’s needs. Mealtime insulin acts within 15-20 minutes and peaks around two-to-four hours after injections.
Concentrated Insulin:
Concentrated insulins deliver larger doses of insulin with less volume per milliliter and decrease the number of injections needed at one time for those who need higher doses of insulin. For example, a U-200 insulin pen only requires half the dose of a U-100 pen because it’s twice as concentrated as U-100 insulin. Concentrated insulin pens come in U-200, U-300 and U-500 pens.
Inhaled Insulin:
Inhaled insulin is used right before or during a meal or used to correct high blood sugar. Its effects are felt rapidly, but this type of insulin is contraindicated in people with lung disease, asthma and pulmonary disease. It’s also not recommended in those who smoke or recently ceased smoking. Patients must take a spirometry test, a test that determines how well your lungs work, before and after starting the use of inhaled insulin therapy.
Can Insulin Be Used with Other Medications?
Yes. Insulin can be combined with other medications. If basal insulin is having a positive impact on fasting blood glucose but A1C remains above target, then another type of injectable such as a GLP-1 is recommended.
Also, when starting combination injection therapy, the Standards of Care recommend the treatment of metformin continue and the use of SFUs and DPP-4 inhibitors are gradually discontinued. TZDs and SGLT-2 inhibitors may help those improve management and reduce the amount of insulin needed in those who are having trouble manage diabetes, even with large doses of insulin.
Finally, as adults with type 2 diabetes get older, it’s important to simplify complex insulin regimens because of a decreased ability in self-management.
Glucagon
It’s also important to know if you’re being prescribed insulin or any other kind of diabetes medication, your risk of experiencing low blood sugarhypoglycemia increases.
To stay prepared for low blood sugar episodes, your health care provider may advise you to keep a snack or fast-acting carbs on hand and provide a prescription for glucagon, a medication that raises your blood sugar to normal levels, for emergency situations.
While there was only one option for decades—and it was complicated to use—there are many new and improved emergency glucagon treatment products available today, including:
- Nasal glucagon – Baqsimi®: This is an emergency glucagon that’s administered through your nose.
- Glucagon pen – Gvoke HypoPen®: This is a premixed glucagon injection that you press against your thigh. The auto-inject device makes it quick and easy to use. It is also available in a prefilled syringe (PFS).
- Glucagon vial & syringe – Gvoke Kit®: This is a premixed glucagon in a vial that comes with a syringe, allowing you to draw up the dose manually and inject it directly into your thigh.
- Glucagon pen – Zegalogue®: Also a premixed glucagon, available as an easy-to-use auto-inject device. It is also available in a prefilled syringe (PFS).
Learn about copay cards and patient assistance programs to get glucagon.
What Should I Ask My Doctor?
If you’re considering different medications to help you manage type 2 diabetes, make sure to speak with your doctor about which medications are best for you and your situation. Take into account the following factors:
- Safety and side effects, including hypoglycemia
- Obtaining a prescription for nasal or auto-injectable glucagon
- Benefits or risks for other health-related issues
- Frequency of dosing
- Cost
Check out our type 2 guides on oral medications and insulin for more information on how they help with type 2 diabetes management.
Key Takeaways on When Medications are Prescribed:
- Metformin is the first line of treatment at diagnosis.
- Because type 2 diabetes is a progressive chronic illness, metformin may work for few years until another kind of medication is recommended, called combination therapy.
- Combination therapy helps patients reach and sustain their glycemic goals.
- Some medications are recommended because they benefit people at high risk of chronic kidney disease and cardiovascular disease.
- Insulin, such as basal (long-acting) insulin, is recommended due to T2D progression, at no fault of the patient. Other insulins available are bolus (meal-time) insulin, concentrated insulin and inhaled insulin.
- Insulin can be combined with other medications such as a GLP-1 if A1C targets no fault of the patient.
- Remember, the use of medication is never the patient’s fault and should never be used as a threat by health care providers.

Author
T'ara Smith, MS, Nutrition Education
T’ara was diagnosed with type 2 diabetes in July 2017 at the age of 25. Since her diagnosis, she focused her academic studies and career on diabetes awareness and living a full life with it. She’s excited to have joined the Beyond Type 1 team to continue her work. Two years later, T'ara discovered she'd been misdiagnosed with type 2 and actually has latent autoimmune diabetes in adults (LADA). Outside the office, T’ara enjoys going to the movies, visiting parks with her dog, listening to BTS and cooking awesome healthy meals. T’ara holds an MS in Nutrition Education from American University.
Related Resources
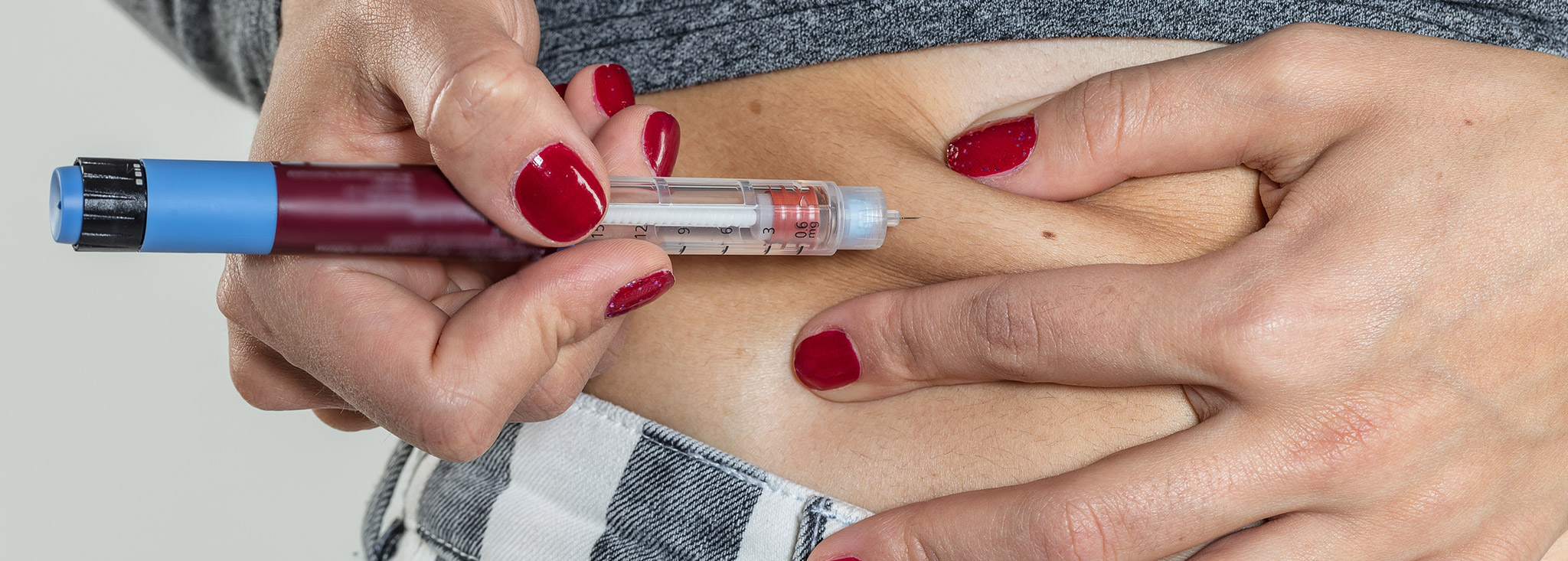
It’s easy to fall into the habit of using the same spot for insulin injections,...
Read more

Managing type 2 diabetes means keeping your blood sugar levels within a healthy range and...
Read more

Physical activity plays a crucial role in managing diabetes, and walking is an easy, effective...
Read more

